Dynamic of disease transmission
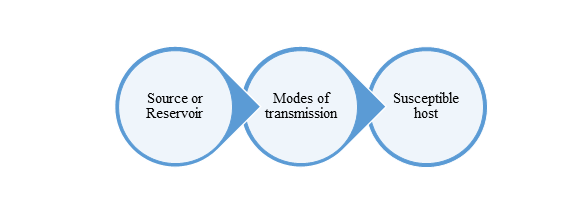
The transmission of communicable diseases involves the transfer of pathogens from the reservoir/source of infection to susceptible hosts. Fundamentally, there are three links in the chain of transmission.

Sources and reservoir
The onset of a communicable disease is initiated by the presence of a reservoir or source of infection. The source of infection is defined as “the person, animal, object, or substance from which an infectious agent passes or is disseminated to the host.” A reservoir is defined as “any person, animal, arthropod, plant, soil, or substance (or a combination of these) in which an infectious agent lives and multiplies, depending primarily on it for survival. It reproduces itself in such a manner that it can be transmitted to a susceptible host.” In summary, the reservoir is the natural habitat where the organism metabolizes and replicates.
The terms reservoir and source are not always interchangeable. For instance, in hookworm infection, the reservoir is man, while the source of infection is the soil contaminated with infective larvae. In typhoid fever, the reservoir of infection may be a case or carrier, whereas the source of infection may include feces or urine of patients, or contaminated food, milk, or water.
The reservoir may be of three types:
- Human reservoir
- Animal reservoir,
- Reservoir in non-living things.
1. Human reservoir
By far, the most significant source or reservoir of infection for humans is humans themselves. They may be cases or carriers.
a. Cases: A case is defined as “a person in the population or study group identified as having the particular disease, health disorder, or condition under investigation.” Various criteria (e.g., clinical, biochemical, laboratory) may be used to identify cases. Broadly, the presence of infection in a host may be clinical, subclinical, or latent.
- The clinical illness may range from mild to moderate, typical to atypical, severe to fatal, depending upon the degree of involvement. Mild cases may be more important sources of infection than severe cases because they are ambulant and can spread the infection wherever they go, whereas severe cases are usually confined to bed.
- Subclinical cases are variously referred to as inapparent, covert, missed, or abortive cases. They are equally important as sources of infection. The disease agent may multiply in the host but does not manifest itself by signs and symptoms. The disease agent is eliminated and contaminates the environment in the same way as clinical cases. Subclinical infection can be detected only by laboratory tests, e.g., recovery of the organism, antibody response, biochemical, and skin sensitivity tests.
- The term latent infection must be distinguished from subclinical infection. In latent infection, the host does not shed the infectious agent, which lies dormant within the host without symptoms (and often without demonstrable presence in blood, tissues, or bodily secretions of the host).
b. Carriers
In certain diseases, either due to inadequate treatment or an insufficient immune response, the infectious agent is not completely eliminated, resulting in a carrier state. A carrier is defined as “an infected person or animal that harbors a specific infectious agent in the absence of discernible clinical disease and serves as a potential source of infection for others.”
Carriers may be classified as below:
A. Type
- lncubatory
- Convalescent
- Healthy
B. Duration
- Temporary
- Chronic
C. Portal of exit
- Urinary
- Intestinal
- Respiratory
- Others
A. By type:
(a) Incubatory carriers: Individuals who shed the infectious agent during the incubation period of the disease, meaning they can infect others before the onset of illness. This typically occurs in the last few days of the incubation period. Examples include measles, mumps, polio, pertussis, influenza, diphtheria, and hepatitis B.
(b) Convalescent carriers: Individuals who continue to shed the disease agent during the convalescence period. Examples include typhoid fever, dysentery (bacillary and amoebic), cholera, diphtheria, and whooping cough. In these diseases, clinical recovery does not necessarily coincide with bacteriological recovery. A convalescent carrier can pose a serious threat to unprotected household members and those in the immediate environment, such as a typhoid fever patient who may excrete the bacilli for 6-8 weeks. This underscores the importance of bacteriological surveillance of carriers after clinical recovery.
(c) Healthy carriers: Healthy carriers arise from subclinical cases. They are individuals who have subclinical infections, developing a carrier state without overt disease but still shedding the disease agent. Examples include poliomyelitis, cholera, meningococcal meningitis, salmonellosis, and diphtheria.
B. By duration:
(a) Temporary carriers: Those who shed the infectious agent for short periods of time. In this category may be included the incubatory, convalescent and healthy carriers.
(b) Chronic carriers: One who excretes the infectious agent for indefinite periods. Chronic carrier state occurs in a number of diseases, e.g., typhoid fever, hepatitis B, dysentery, cerebra-spinal meningitis, malaria, gonorrhea, etc. Chronic carriers are far more important sources of infection than cases. The longer the carrier state, the greater the risk to the community. The duration of the carrier state varies with the disease. In typhoid fever and hepatitis B, the chronic carrier state may last for several years; in chronic dysentery, it may last for a year or longer.
C. By portal of exit:
Carriers may also be classified according to the portal of exit of the infectious agent. Thus, we have urinary carriers, intestinal carriers, respiratory carriers, nasal carriers, etc. Skin eruptions, open wounds, and blood are also portals of exit. In the case of typhoid fever, a urinary carrier is more dangerous than an intestinal carrier.
2. Animal reservoir
The source of infection may sometimes be animals and birds. Similar to human sources of infection, these animals and birds may be cases or carriers. The diseases and infections that are transmissible to humans from vertebrates are called zoonoses. There are over 100 zoonotic diseases that may be transmitted to humans from animals and birds. Well-known examples include rabies, yellow fever, and influenza.
3. Reservoir in non-living things
Soil and inanimate matter can also serve as reservoirs of infection. For example, soil may harbor agents that cause tetanus, anthrax, etc.
Modes of transmission
Communicable diseases can be transmitted from the reservoir or source of infection to a susceptible individual in various ways, depending on the infectious agent, portal of entry, and local ecological conditions. Generally, an infectious disease is transmitted through a single route, for example, typhoid fever through vehicle transmission and the common cold through direct contact. However, there are diseases that can be transmitted through multiple routes, such as AIDS, salmonellosis, hepatitis B, etc. The existence of multiple transmission routes enhances the survival of the infectious agent. The modes of transmission of infectious diseases can be classified as follows.
A. Direct transmission.
- Direct contact: Infection may be transmitted by direct contact from skin to skin, mucosa to mucosa, or mucosa to skin of the same or another person. This implies direct and essentially immediate transfer of infectious agents from the reservoir or source to a susceptible individual, without an intermediate agency. Examples include skin-to-skin contact through touching, kissing, or sexual intercourse, and continued close contact. Direct contact not only reduces the period for which the organism will have to survive outside the human host but also ensures a larger dose of infection. Diseases transmitted by direct contact include STD and AIDS, leprosy, leptospirosis, skin and eye infections.
- Droplet infection: This involves the direct projection of a spray of droplets of saliva and nasopharyngeal secretions during coughing, sneezing, or speaking. The expelled droplets may impinge directly upon the conjunctiva, oro-respiratory mucosa, or skin of a close contact. Diseases transmitted by droplet spread include many respiratory infections, eruptive fevers, many infections of the nervous system, common cold, diphtheria, whooping cough, tuberculosis, meningococcal meningitis, etc. The potential for droplet spread is increased in conditions of close proximity, overcrowding, and lack of ventilation.
- Contact with soil: The disease agent may be acquired by direct exposure of susceptible tissue to the disease agent in soil, compost, or decaying vegetable matter in which it normally leads a saprophytic existence (e.g., hookworm larvae, tetanus, mycosis, etc.).
- Inoculation into skin or mucosa: The disease agent may be inoculated directly into the skin or mucosa (e.g., rabies virus by dog bite, hepatitis B virus through contaminated needles and syringes).
- Transplacental (or vertical) transmission: Disease agents can be transmitted transplacentally. This is another form of direct transmission. Examples include the so-called TORCH agents (Toxoplasma gondii, rubella virus, cytomegalovirus and herpes virus), varicella virus, syphilis, hepatitis B, and AIDS. Some of the non-living agents as drugs can also be transmitted vertically. In these cases, the disease agent produces malformations of the embryo by disturbing its development.
B. Indirect transmission
Indirect transmission embraces various mechanisms, including the traditional 5 F’s – “flies, fingers, fomites, food, and fluid.” An essential requirement for indirect transmission is that the infectious agent must be capable of surviving outside the human host in the external environment and retain its basic properties of pathogenesis and virulence until it finds a new host. Indirect transmission can occur in various settings.
1. Vehicle-borne: Vehicle-borne transmission implies the transmission of the infectious agent through the agency of water, food (including raw vegetables, fruits, milk and milk products), ice, blood, serum, plasma or other biological products such as tissues and organs. Of these water and food are the most frequent vehicles of transmission, because they are used by everyone. The infectious agent may have multiplied or developed in the vehicle (e.g., S. aureus in food) before being transmitted; or only passively transmitted in the vehicle (e.g., hepatitis A virus in water}. Diseases transmitted by water and food include chiefly infections of the alimentary tract, e.g., acute diarrhoeas, typhoid fever, cholera, polio, hepatitis A, food poisoning and intestinal parasites. Those transmitted by blood include hepatitis B, malaria, syphilis etc.
2. Vector-borne: In infectious disease epidemiology, a vector is defined as an arthropod or any living carrier (e.g., snail) that transports an infectious agent to a susceptible individual. Transmission by a vector may be mechanical or biological. Diseases transmitted by vectors include those carried by arthropods such as flies, mosquitoes, fleas, cockroaches, lice, bugs, ticks, and mites, as well as vertebrates like mice, rodents, and bats.
Epidemiological classification of vector-borne diseases
I. By vector
a) Invertebrate type: Arthropod vectors fall into seven orders largely
- Diphtheria – flies and mosquitoes
- Siphonaptera- fleas
- Orthoptera- cockroaches
- Anoplura – sucking lice
- Hemiptera – bugs, including kissing bugs
- Acarina– ticks and mites
- Copepoda – cyclops
b) Vertebrate type – Mice, rodents, bats.
II. By transmission chain
Vector-borne diseases are classified under heterogeneous infection chain and involve three principle patterns:
a) Man and a non-vertebrate host
- Man-arthropod-man (malaria)
- Man-snail-man (schistosomiasis).
b) Man, another vertebrate host, and a non-vertebrate host
- Mammal-arthropod-man (plague)
- Bird-arthropod-man (encephalitis).
c) Man and 2 intermediate hosts
- Man-cyclops-fish-man (fish tape worm)
- Man-snail-fish-man (Clonorchissinensis)
- Man-snail-crab-man (Paragonimiasis).
III. By methods in which vectors transmit agent
- Biting
- Regurgitation
- Scratching-in of infective faeces
- Contamination of host with body fluids of vectors.
IV. By methods in which vectors are involved in the transmission and propagation of parasites
- Mechanical transmission: The infectious agent is mechanically transported by a crawling or flying arthropod through soiling of its feet or proboscis; or by passage of organisms through its gastrointestinal tract and passively excreted. There is no development or multiplication of the infectious agent on or within the vector.
- Biological transmission: The infectious agent undergoing replication or development or both in vector and requires an incubation period before vector can transmit. Biological transmission is of three types: (i) Propagative: The agent merely multiplies in vector, but no change in form, e.g., plague bacilli in rat fleas. (ii) Cyclo-propagative: The agent changes in form and number, e.g., malaria parasites in mosquito. (iii) Cyclo-developmental: The disease agent undergoes only development but no multiplication, e.g., microfilaria in mosquito.
3. Airborne
- Droplet nuclei: “Droplet nuclei” are a type of particles implicated in the spread of airborne infection. They are tiny particles (1-10 microns range) that represent the dried residue of droplets. They may be formed by (a) evaporation of droplets coughed or sneezed into the air or (b) generated purposefully by a variety of atomizing devices (aerosols). The droplet nuclei may remain airborne for long periods of time. Particles in the 1-5-micron range are liable to be easily drawn into the alveoli of the lungs and may be retained there. Diseases spread by droplet nuclei include tuberculosis, influenza, chickenpox, measles and many respiratory infections. Mention must also be made of the role of airborne spread of toxic air pollutants including “smog” resulting in air pollution epidemics.
- Dust: Some of the larger droplets which are expelled during talking, coughing or sneezing, settle down on the floor, carpets, furniture, clothes, bedding, linen and other objects in the immediate environment and become part of the dust. A variety of infectious agents are found in the dust of hospital wards and living rooms. Some of them (e.g., tubercle bacilli) may survive in the dust for considerable periods under optimum conditions of temperature and moisture. During the act of sweeping, dusting and bed-making, the dust is released into the air and becomes once again airborne. Other diseases carried by infected dust include streptococcal, staphylococcal infection, pneumonia and tuberculosis etc. Airborne dust is primarily inhaled, but may settle on uncovered food and milk. This type of transmission is most common in hospital-acquired (nosocomial) infection.
4. Fomite-borne
Fomites (singular; fomes) are inanimate articles or substances other than water or food contaminated by the infectious discharges from a patient and capable of harboring and transferring the infectious agent to a healthy person. Fomites include soiled clothes, towels, linen, handkerchiefs, cups, spoons, pencils, books, toys, drinking glasses, door handles, taps, lavatory chains, syringes, instruments and surgical dressings. The fomites play an important role in indirect infection. Diseases transmitted by fomites include diphtheria, typhoid fever, bacillary dysentery, hepatitis A, eye and skin infections.
5. Unclean hands and fingers
Hands are the most common medium by which pathogenic agents are transferred to food from the skin, nose, bowel, etc. as well as from other foods. The transmission takes place both directly (hand-to-mouth) and indirectly. Examples include staphylococcal and streptococcal infections, typhoid fever, dysentery, hepatitis A and intestinal parasites. Unclean hands and fingers imply lack of personal hygiene.
Susceptible host
The susceptibility of a host to infectious diseases involves four stages:
- First, infectious agent must find a portal of entry by which it may enter the host. There are many portals of entry, e.g., respiratory tract, alimentary tract, genitourinary tract, skin, etc. Some organisms may have more than one portal of entry, e.g., hepatitis B, brucellosis.
- On gaining entry into the host, the organisms must reach the appropriate tissue or “site of selection “in the body of the host where it may find optimum conditions for its multiplication and survival.
- Thirdly, the disease agent must find a way out of the body portal of exit in order that it may reach a new host and propagate its species. If there is no portal of exit, the infection becomes a dead-end infection as in rabies, bubonic plague, tetanus.
- After leaving the human body, the organism must survive in the external environment for sufficient period till a new host is found. In addition, a successful disease agent should not cause the death of the host but produce only a low-grade immunity so that the host is vulnerable again and again to the same infection. The best example is common cold virus.
Sources: Park, K. (2021). Park’s Textbook of Preventive and Social Medicine (26th ed.). Bhanot Publishers.
Additional link: Click here